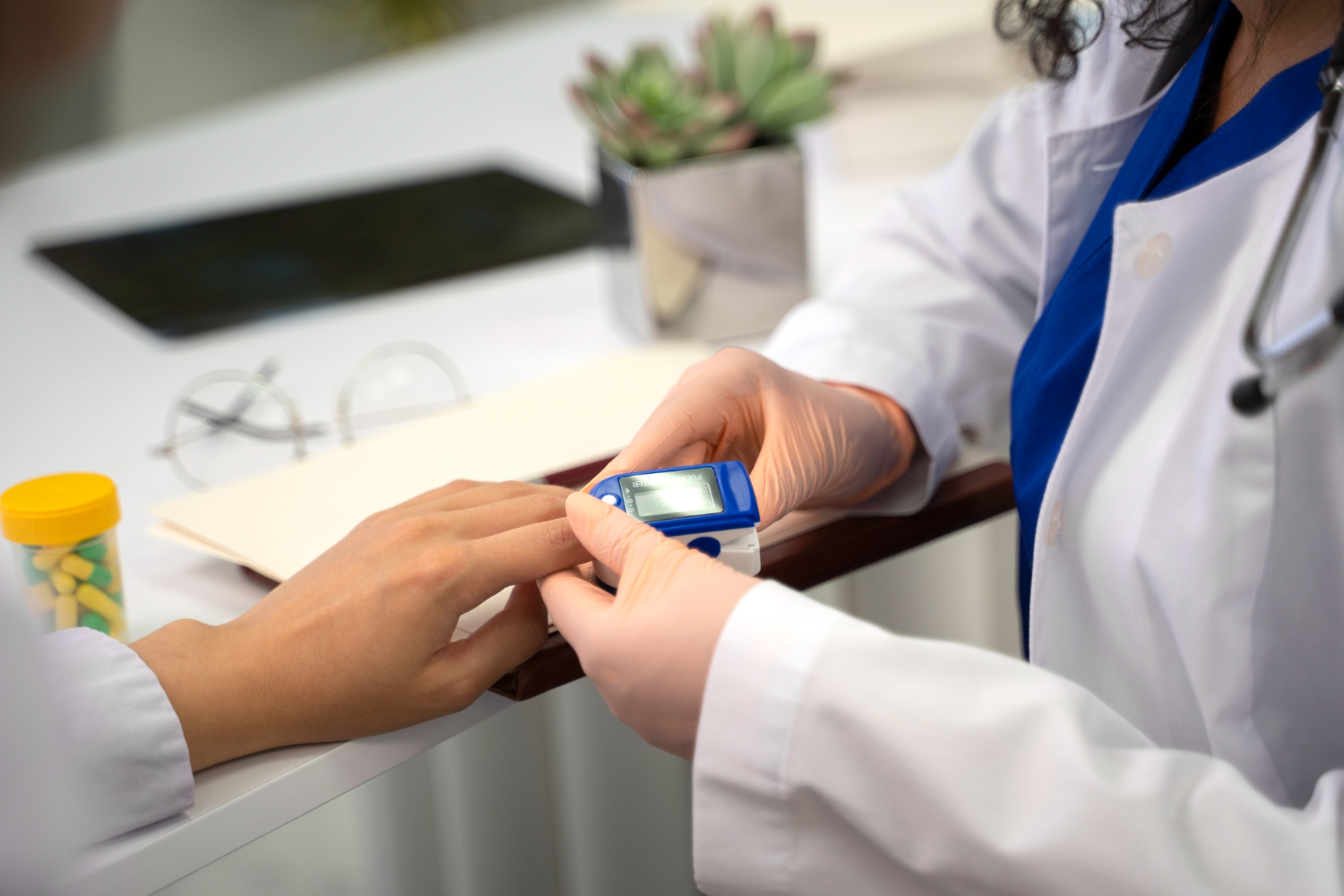
Managing diabetes successfully requires teamwork — not just medication and daily routines, but clear communication with the healthcare professionals supporting you. Your doctor and pharmacist play vital roles in shaping your diabetes treatment plan, adjusting it over time, and helping you stay confident in your self-care.
Many people, however, attend appointments unsure about what to ask. This guide uses a friendly Q&A style to help you understand what to discuss, how to communicate effectively, and how to get the most out of your diabetes care. At Diabetes Pharmacy, we believe informed patients make stronger decisions — and this guide is designed to help you do exactly that.
1: Understanding Your Diagnosis and Long-Term Plan
Q: I’ve been diagnosed with diabetes — how do I understand what that means for me?
Your doctor should explain whether you have type 1 or type 2 diabetes, how it affects your body, and what steps you need to take to stay healthy. Ask them to clarify anything you’re unsure about — from how insulin works to how your pancreas behaves. There’s no such thing as a silly question.
Q: What should I ask during my first or annual diabetes review?
Start with your current numbers. Ask:
- “What is my HbA1c, and what should my target be?”
- “Has anything changed since my last review?”
Your doctor can explain whether your levels are improving or need attention. This helps you understand how well your plan is working.
Q: What symptoms should I never ignore?
Ask your doctor to list red-flag symptoms such as unusual thirst, blurred vision, tingling in feet, or sudden drops in blood sugar. Knowing what to look for helps prevent long-term complications.
2: Asking the Right Medication Questions
Q: I take diabetes medication, but I don’t always understand what each one does. What should I ask?
Ask your doctor to explain each medication in simple terms.
For example:
- “What does this medication do?”
- “How does it help my body use insulin?”
- “When should I take it — with meals, before bed, or at specific times?”
This helps you use your medication correctly and confidently.
Q: How do I know if my medication needs adjusting?
If you experience frequent highs or lows, new symptoms, changes in appetite or weight, or your HbA1c rises, speak up. Your doctor may adjust your dose or recommend a different medication. Treatment plans change — it’s normal.
Q: Should I ask about side effects?
Absolutely. Ask:
- “What side effects are normal?”
- “Which ones should I report immediately?”
Your pharmacist can also answer these questions and guide you on safe usage.
Q: What if my medications aren’t working well enough?
Your doctor might suggest adding another medication or moving to insulin. They may also recommend improved monitoring through tools like the FreeStyle Libre 2 Plus to better understand your glucose patterns.
3: Monitoring Questions (Glucometers, CGM & Frequency)
Q: How often should I be checking my blood sugar?
This depends on your treatment plan. People on insulin or certain tablets may need to check multiple times a day, while others may need one or two checks. Ask your doctor:
- “What monitoring routine suits my medication and lifestyle?”
Q: Should I consider a continuous glucose monitor (CGM)?
If your levels fluctuate frequently, if you struggle to spot lows, or if finger-pricks feel difficult, a CGM could help. Ask:
- “Would a CGM give me clearer insights into my glucose patterns?”
Doctors often recommend CGM for patients who want more accurate, real-time information. You can explore CGM options such as the FreeStyle Libre 2 Plus for continuous tracking with no routine finger-pricks.
Q: What should I look for when reviewing my glucose readings?
Ask your doctor or pharmacist to help you understand trends like morning highs, post-meal spikes or unusually low readings. Monitoring becomes far more effective when you know how to interpret patterns.
4: Questions About Diet, Exercise & Lifestyle
Q: What should I ask my doctor about food?
Diet is deeply personal. Ask questions like:
- “How do different carbs affect my glucose?”
- “Should I work with a dietitian?”
- “Are there foods I should limit based on my medication?”
Your doctor can explain how to balance meals and manage portion sizes without feeling restricted.
Q: What about exercise — how do I know what’s safe?
Movement is hugely beneficial for diabetes, but ask:
- “What exercises are suitable for my age and fitness level?”
- “Will exercise make my glucose drop?”
- “Do I need to adjust my medication before activity?”
If you use a CGM like the FreeStyle Libre 2 Plus, it can show how activity affects your glucose in real time.
Q: Should I discuss stress, sleep or mental health as well?
Yes — emotional well-being affects blood sugar. If stress or sleep issues are affecting your routine, discuss them openly. Diabetes care isn’t only physical.
5: What to Ask Your Pharmacist (Often Overlooked)
Q: How can my pharmacist help with my diabetes plan?
More than you might expect. Your pharmacist ensures you understand your medication, checks for interactions, reminds you about proper use and can guide you with general care tips.
Q: What specific questions should I ask my pharmacist?
Try these:
- “Can you show me how to use my insulin or pen correctly?”
- “Is it safe to take this over-the-counter medicine with my diabetes tablets?”
- “How should I store my medication while travelling?”
- “Which monitoring tools would you recommend?”
Pharmacists at Diabetes Pharmacy can also help you choose the right supplies and explain how to use CGM sensors effectively.
Q: Can I ask my pharmacist about foot care or skin issues?
Yes — pharmacists can advise on minor wounds, dry skin, foot concerns and when to seek medical help.
6: Reviewing and Updating Your Diabetes Plan
Q: How often should I review my diabetes plan?
At least once a year — but sooner if your glucose changes, medication stops working well, or lifestyle adjustments aren’t helping. Ask your doctor:
- “Is my current plan still the best option for me?”
Q: What should I discuss during a review?
Talk about new symptoms, daily challenges, changes in activity or diet, and your glucose trends. Use your readings or CGM data to guide the conversation.
Q: How do I know when my plan needs updating?
If you’re experiencing frequent highs or lows, or your HbA1c is rising, your doctor may suggest new medications or updated monitoring systems.
Support from Diabetes Pharmacy
Your healthcare team is there to guide you — and so are we. At Diabetes Pharmacy, you can explore trusted diabetes supplies through our convenient online shop, including the latest CGM sensors such as the FreeStyle Libre 2 Plus.
If you want to learn more about our mission, visit our About Us page. If you have questions about supplies or need personalised support, reach out through our Contact Us page. For more guides like this one, explore our blog section.
Final Thoughts
Working effectively with your doctor and pharmacist is one of the strongest ways to improve your diabetes care. Asking questions — even small ones — helps you understand your body, your treatment and your daily routine. With open communication and the right tools from Diabetes Pharmacy, you can build a diabetes plan that feels personalised, safe and empowering.