Blood Glucose Meters Without Test Strips: Are They Worth It?
For many people living with diabetes, blood glucose testing is part of everyday life. While traditional finger-prick testing using individual test strips is reliable, it can also feel repetitive, messy, and inconvenient — especially when testing several times a day.
This has led many people to search for blood glucose meters without test strips, hoping for a simpler and more discreet way to manage blood sugar levels. But are strip-free blood glucose meters really worth it, or are traditional systems still the better option?
In this guide, we explain how strip-free blood glucose testing works, who benefits most, what the limitations are, and how to decide which monitoring method suits your lifestyle.
At Diabetes Pharmacy, we help people across the UK choose blood glucose monitoring solutions that are practical, reliable, and easy to live with.
Why People Are Looking for Blood Glucose Meters Without Test Strips
Traditional blood sugar testing requires several separate items: a meter, test strips, lancets, and a disposal method for used strips. While this works well, it can feel inconvenient over time.
Many users find that:
- Handling small test strips can be awkward
- Testing in public feels uncomfortable
- Carrying multiple supplies is inconvenient
- Disposing of used strips isn’t always easy
These daily frustrations are why interest in glucometers without test strips has grown steadily in recent years.
What Are Blood Glucose Meters Without Test Strips?
Blood glucose meters without test strips are devices designed to test blood sugar without inserting a new strip for each test. Instead of loose strips, they use an internal testing system, usually in the form of a cassette.
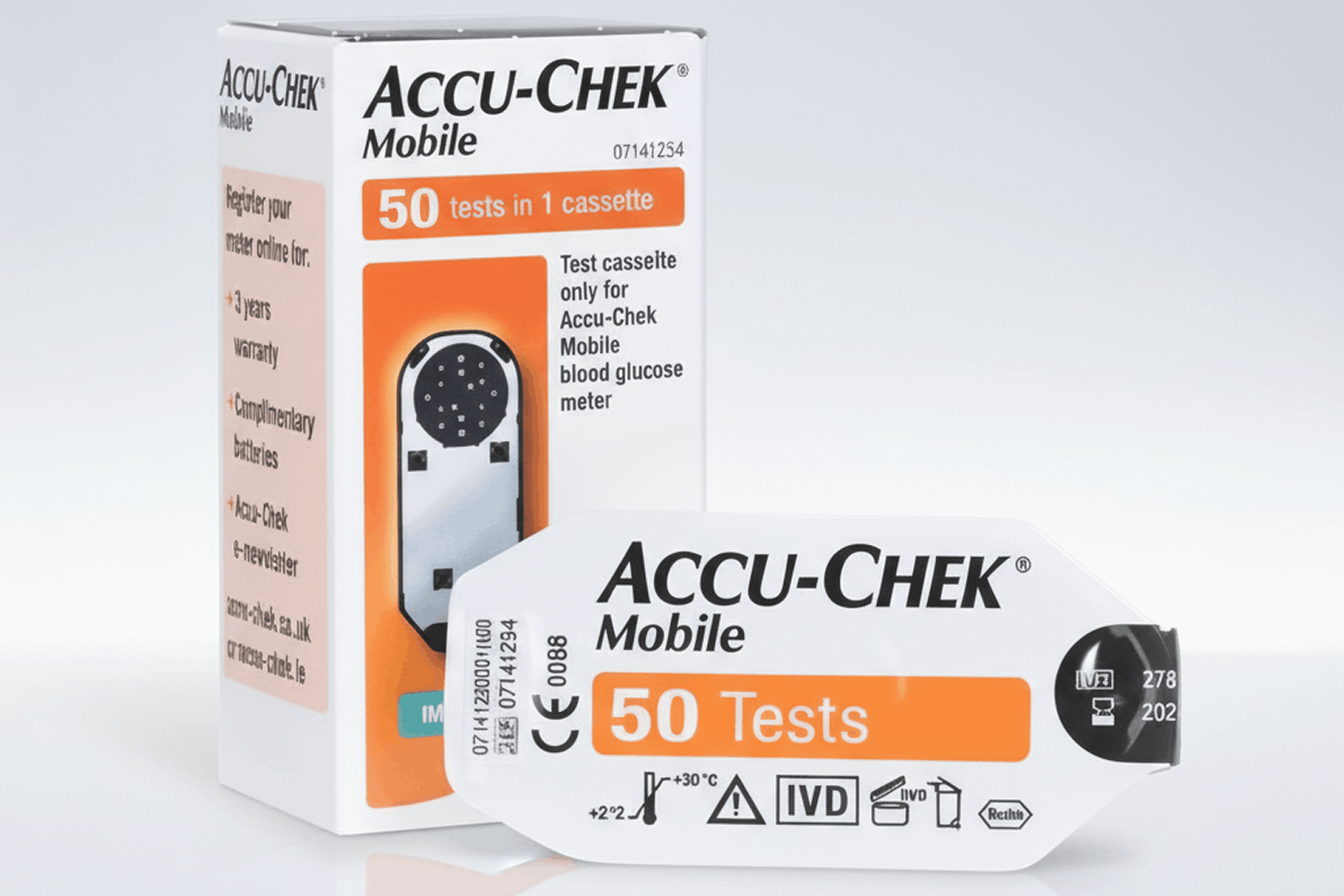
The most well-known example in the UK is the Accu-Chek Mobile system, which uses a cassette containing 50 tests rather than individual strips. The cassette stays inside the meter and advances automatically after each test.
This approach removes the need to handle, insert, and dispose of strips, making strip-free blood sugar testing simpler for many users.
You can view the compatible cassette here: Accu-Chek Mobile Test Cassette – 50 Tests
How Strip-Free Blood Sugar Testing Works
With a strip-free blood glucose meter, testing follows a similar finger-prick process — but without inserting a strip.
Instead, the device:
- Uses a built-in lancing device to collect a small blood sample
- Applies the blood to a fresh section of the internal cassette
- Measures your blood glucose level
- Seals away the used test area automatically
Because the cassette contains multiple tests, everything stays contained within the meter. This significantly reduces handling and helps keep testing more discreet and hygienic.
Advantages of Blood Glucose Meters Without Test Strips
The biggest benefit of strip-free blood glucose meters is convenience. By simplifying the testing process, many users find it easier to stay consistent with monitoring.
Key advantages include:
- Less mess and waste compared to loose strips
- Faster testing, especially when out of the house
- All-in-one design with fewer items to carry
- Discreet testing in public or work settings
For people who test frequently, these small improvements can make daily diabetes management feel far less disruptive.
Are There Any Drawbacks to Strip-Free Blood Glucose Meters?
While strip-free systems offer clear benefits, they are not perfect for everyone. Understanding the limitations helps you make a confident choice.
Some considerations include:
- Fewer device options compared to traditional meters
- You must replace the cassette after a fixed number of tests
- You cannot mix and match with other test strips
- They may not suit people who already rely heavily on CGM
Being honest about these points builds trust — and helps ensure you choose a system that fits your routine.
Who Are Blood Glucose Meters Without Test Strips Worth It For?
Strip-free blood glucose testing tends to work best for people who value simplicity and convenience.
These systems are often ideal for:
- People testing blood sugar multiple times a day
- Older adults who struggle with small test strips
- People with reduced dexterity or vision
- Travellers who want fewer loose supplies
- Anyone frustrated by traditional strip handling
If convenience is a priority, a glucometer without test strips can be a worthwhile upgrade.
How Do Strip-Free Meters Compare to Traditional Test Strip Systems?
Traditional blood glucose meters using strips remain extremely popular — and for good reason. They offer flexibility, wide availability, and compatibility with many different strip brands.
Popular strip-based systems include:
- GlucoRx S HCT Blood Glucose Meter
- Kinetik Wellbeing Glucose Test Strips
- GlucoRx HCT Glucose Test Strips
- MyLife Pura Glucose Test Strips
- Accu-Chek Active Test Strips
- Contour Test Strips – Pack of 50
These systems are reliable and often more affordable per test. However, they require more handling and supplies compared to strip-free alternatives.
Ultimately, the choice comes down to flexibility versus convenience.
Are Strip-Free Blood Glucose Meters Worth It in the UK?
For UK users, strip-free blood glucose meters are absolutely worth considering — especially if you test frequently and value simplicity.
Availability of replacement cassettes, trusted suppliers, and consistent access to supplies all play an important role. Buying from a reliable UK retailer ensures continuity and peace of mind.
Through the Diabetes Pharmacy online shop, UK customers can access strip-free testing supplies, traditional meters, and compatible test strips in one place.
How to Decide Which Blood Glucose Monitoring System Is Right for You
Choosing between blood glucose meters with or without test strips depends on your daily routine, not just technology.
Ask yourself:
- How often do I test my blood sugar?
- Do I find handling strips frustrating?
- Do I test at work, while travelling, or in public?
- Do I prefer simplicity over flexibility?
- Am I already using CGM regularly?
Answering these questions honestly will guide you toward the system you’re most likely to use consistently.
If you’d like help discussing monitoring options with your healthcare provider, our guide on how to work with your doctor and pharmacist explains how to approach the conversation confidently.
Final Thoughts: Are Blood Glucose Meters Without Test Strips Worth It?
Blood glucose meters without test strips are not a universal replacement for traditional systems — but for the right person, they can make a meaningful difference.
If you test frequently, value convenience, and want to simplify daily monitoring, strip-free blood sugar testing can be well worth it. For others who prioritise flexibility or already use CGM, traditional test strip systems may still be the better choice.
With trusted products, clear guidance, and ongoing support from Diabetes Pharmacy, choosing the right blood glucose monitoring system becomes simpler, calmer, and far more confident.